Duration: 01 September 2019 - 30 September 2023
Funder: Arthritis UK
Chief investigator: Dr Rosemary Hollick
Other UoA investigators: Professor Corri Black (Aberdeen Centre for Health Data Science), Professor Louise Locock (Health Services Research Unit)
Other co-investigators: Dr Neil Basu (University of Glasgow), Professor Mark Little (Trinity College, Dublin)
Individuals with rare rheumatic diseases report an uphill struggle to navigate healthcare systems not designed to manage complex diseases. Whilst delays in receiving a diagnosis, inconsistent access to relevant expertise and uncoordinated care are not unique to rare rheumatic disease, the consequences in this group of individuals can be devastating.
A good example is systemic vasculitis, a group of devastating but treatable multi-organ illnesses caused by inflammation of the blood vessels. Across the UK there are significant differences in how these conditions are looked after. Our own pilot data from a selection of specialist centres also reveals clinically important differences in outcomes such as heart disease, stroke and infections. There is increasing momentum within the UK to implement commitments made in the UK Rare Disease Strategy, and within Europe to improve services for those with rare diseases. However, there are currently no robust studies to help us decide how best to organise and deliver services for those with adult onset rare rheumatic disease.

Further information
- What were the aims of this research?
-
This study set out to understand which key elements of care delivery are associated with health outcomes of prime importance to individuals with vasculitis. This information enables us to advise on better service design for people living with vasculitis, and help to ensure more equitable access to effective, coordinated care and support.
Specifically aimed to identify key components underpinning good care; explore the link between key service components and individual health outcomes; and examine the barriers and facilitators to implementing service components in practice.
This was done by several investigatory methods, including:
- a multi-professional survey of vasculitis service providers across the UK and Ireland
- interviews with patients with various forms of vasculitis
- organisational case studies and interviews with healthcare professionals who provide vasculitis services
- analysis of national routinely collected healthcare datasets
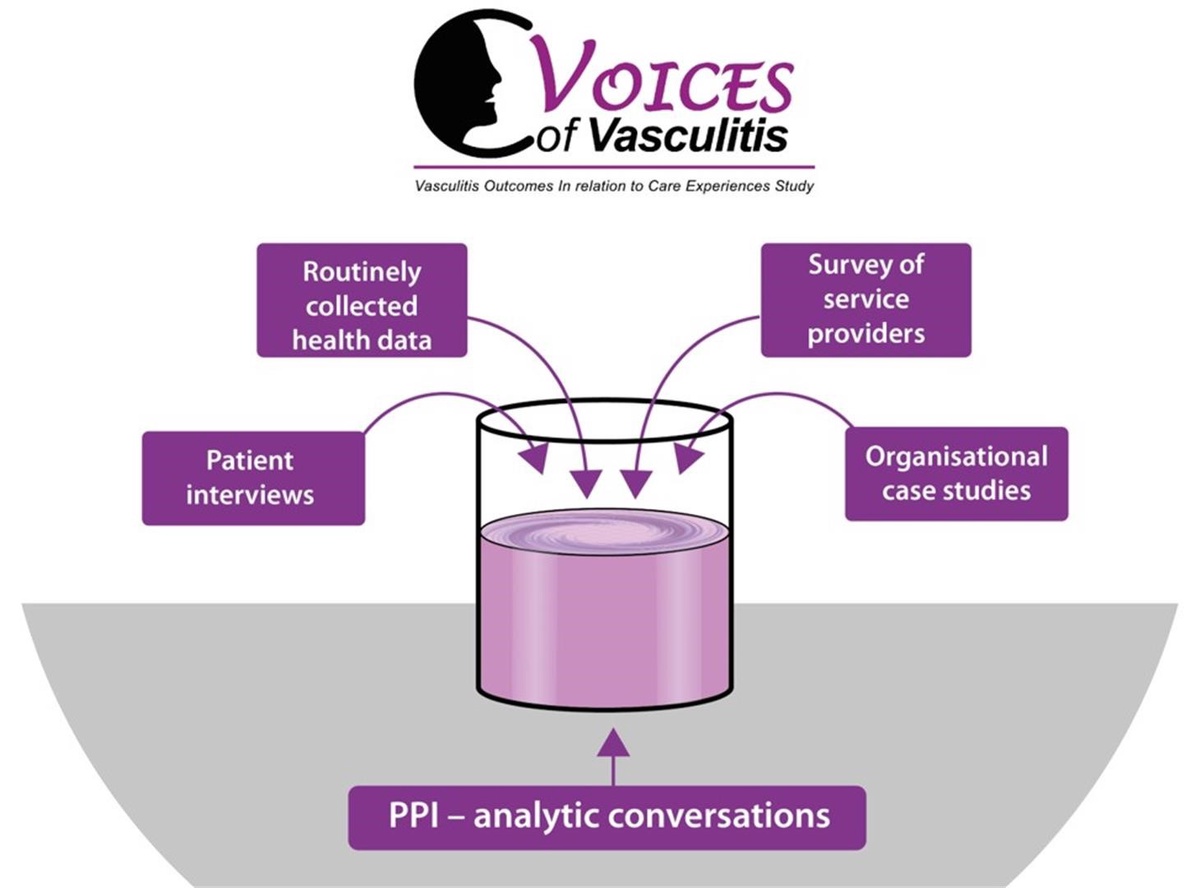
Patients also played a key role in the VOICES project, describing their experience of care and working with us to create impactful outputs grounded in patient experience.
- How will this research benefit patients?
-
By the end of this study we will have developed, in conjunction with patients, healthcare professionals and decision makers, a timely set of recommendations that will directly inform policy decisions on how to improve services for patients with rare diseases. We will use our learning from patient interviews to develop an accessible online information resource for people with systemic vasculitis, their families and carers in collaboration with the University of Oxford and the Health Experience Insights website team (Systemic Vasculitis - Overview (ox.ac.uk) ).
- What did the study find, and what have we done with this information so far?
-
Ultimately the results of the VOICES study will enable us, in conjunction with patients, healthcare professionals and decision makers, to produce a timely set of recommendations that will directly inform policy decisions on how to improve services for patients with rare diseases, and have also used learning from patient interviews to develop an accessible online information resource for people with systemic vasculitis, their families and carers in collaboration with the University of Oxford and the Health Experience Insights website team (which can be found here).
The study has produced the following outputs so far:
American College of Rheumatology: Convergence 2024
Washington DC, USA: 14 - 19 November 2024
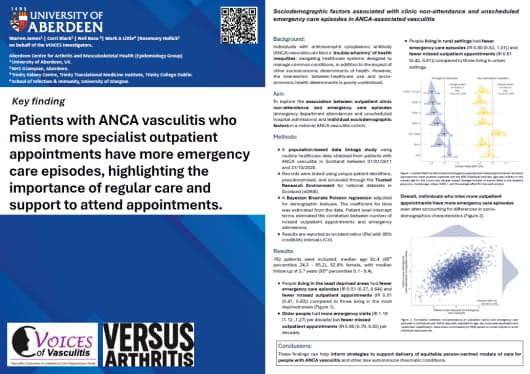
Dr Rosemary Hollick presented a poster at this event on the sociodemographic factors which are associated with non-attendance at clinical appointments and unscheduled emergency care episodes for people with ANCA-associated vasculitis. You can view Dr Hollick's poster below.
- Warren James, Corri Black, Neil Basu, Mark Little and Rosemary Hollick on behalf of the VOICES investigators. Sociodemographic Factors Associated with Clinic Non-attendance and Unscheduled Emergency Care Episodes in ANCA-associated Vasculitis [poster presentation]
Summary report to funders
During a recent visit to the Epidemiology Group premises at Foresterhill Campus, we were delighted to present our latest research findings to one of our key funding partners, Arthritis UK (formerly Versus Arthritis) . As part of these presentations, we produced a poster from the VOICES study summarising our key findings.
You can view and download the poster below:
- Hollick, James, Nicoll, Locock, Black, Dhaun, Egan, Fluck, Laidlaw, Lanyon, Little, Luqmani, Moir, McBain and Basu, We have identified key parts of health care services that improve experiences and health outcomes for people with vasculitis
.jpg)
Improving care delivery for people with rare conditions
Dr Rosemary Hollick and Lynn Laidlaw delivered a presentation at Health Services Research UK Conference 2024 incorporating results from the VOICES study, with recommendations for how we can improve care delivery for people with rare conditions such as systemic vasculitis.
You can watch a full video of the presentation below:
Latest paper from the VOICES study
Our paper summarising the findings from the VOICES study has now been published in The Lancet Rheumatology, and is available here:
This is the first study to identify key components of an optimal rare rheumatic disease health care service, grounded in patient and provider experiences. We have evidenced that these components are significantly associated with improved health outcomes, employing national population level administrative data, and have identified underpinning factors to inform initiatives to improve the design, delivery, and effectiveness of health-care models for rare autoimmune rheumatic diseases.
A Plain Language Summary of this paper is also available here.
_-_Thumbnail.jpg)
We have produced a companion infographic which captures some of the key features of this research and its findings:

You can download a copy of the infographic here .
There is a related podcast with The Lancet Rheumatology in conversation with Dr Rosemary Hollick, which you can listen to here:
- 'In conversation with... Rosemary Hollick' - The Lancet Rheumatology Podcast (you can also download the podcast here )
You can read a press release announcing the results of the study here:
- New study shows how to improve health outcomes and care for thousands living with rare conditions - University of Aberdeen, SMMSN News, 21 May 2024
Stop ticking boxes: it just doesn't work
In this piece, which accompanies our recent paper from the VOICES study (see above), public contributors Lynn Laidlaw and Mo McBain discuss their frustrations in trying to navigate healthcare systems which are not designed to support people with complex rare autoimmune conditions such as systemic vasculitis.

You can read the full article here (free sign-up required)
Blog post: Versus Arthritis - 'How our research is improving care for rare conditions like vasculitis'
To mark Rare Diseases Day 2024, Versus Arthritis put the spotlight on vasculitis. Click on the link below to see and hear how our VOICES study is improving care for rare conditions like vasculitis.
Moving beyond aspirational rhetoric - learning from the role of professional jurisdictions in integrated care delivery in rare disease
Dr Rosemary Hollick has recorded the following presentation for the upcoming Health Services Research UK Conference 2023 . You can watch a full video of Dr Hollick's talk below:
Voicing experience to improve care for people with rare autoimmune conditions
In July 2022, the team gave a presentation at the Health Services Research UK Conference 2022. You can see our full recorded presentation below.
We filmed a conversation we had about how we work together, the productive tensions we experience, and the trusting relationships we try to build. We framed our conversation by thinking about the ethic of responsibility we have to each other, to other patients, to our NHS colleagues, and to the quality of the research.
We were delighted to win an Innovation in Inclusion in Health Services Research award, supported by the Health Services Research National Specialty Group in the NIHR Clinical Research Network. You can read more about this in an accompanying blog - Frankly speaking - conversations about PPI - where Louise Locock reflects on our experiences.'
Developing a website resource through qualitative research into experiences of systemic vasculitis and UK healthcare
The ANCA 2022 conference in Dublin (April 2022) brought together key clinicians and researchers in the field of ANCA-associated vasculitis. As this was an important opportunity to publicise the VOICES systemic vasculitis web resource and catalyst film to clinicians, we put together this poster about how we developed the resource , what it includes, and how people can use it in their clinical practice
.jpg)
Experiences of systemic vasculitis and UK healthcare
This web resource on Health Experience Insights (Systemic Vasculitis - Overview (ox.ac.uk) ) - part of our qualitative research - features 32 people from across the UK talking about what it's like to live with systemic vasculitis.
Supporting conversations about healthcare improvement
This short film is from our interviews with people across the UK who live with systemic vasculitis. We hope it will help staff and patients think about how they could improve care locally.

Doing online remote interviews (podcast)
This 10-minute audio reflective conversation (accompanied by 4 slides) includes VOICES researcher Avril Nicoll and patient partner and participant Lynn Laidlaw. It was presented at DIPEx 2020, an international meeting of qualitative researchers interested in people's experiences of health conditions and healthcare.
You can download the podcast. Accompanying slides are available at this link.
"So Many Limits": Living with Subglottic Stenosis as a Result of Vasculitis
This poster presentation gives an overview of Charlie Harper's experiences of living with communication and swallowing problems as a results of systemic vasculitis.

You can download a PDF version of the poster here .
- Warren James, Corri Black, Neil Basu, Mark Little and Rosemary Hollick on behalf of the VOICES investigators. Sociodemographic Factors Associated with Clinic Non-attendance and Unscheduled Emergency Care Episodes in ANCA-associated Vasculitis [poster presentation]
- Patient and public involvement
-
Patient Partner stories
Our Patient Partners have kindly shared some of their experiences of living with vasculitis:
Mo's story
"As a patient with vasculitis, but also having worked as nurse and researcher, I knew how important this study would be and the difference it could make, so I was more than happy to have “my voice” heard.

Due to the fact that different groups' perspectives (professionals and patients) have been listened to, this study will for the first time give a clearer picture of what patients are experiencing regarding access to treatment and support services and more importantly suggestions on what and where improvements could be made.
For me, this project is proof that we (as patients) have been included and that our voices are being heard. Saying that, there is still much work to be done regarding awareness, research, education and support into vasculitis but hopefully this project will fill some of these gaps and I'm looking forward to seeing the outcomes."
The value of research - and being a patient advisor - Steve Chinn
I was diagnosed with ANCA Vasculitis with MPO Antibodies, also known as Microscopic Polyangiitis, in December 2018. With hindsight, I can see that my health had been declining for some time: I was getting more fatigued when walking, and had signs of kidney problems. Within a year, the vasculitis had removed all of my kidney function, and caused significant scarring in my lungs. I am now a dialysis patient, and am on a cocktail of treatments to keep the vasculitis in remission, and try to stop further damage to the lungs. But as we all know, this disease can progress, so the future is uncertain.

So I try to give something back by acting as a patient advisor on research projects. This involves working with the research team to build a patient perspective into the way research needs are identified, and the research itself is designed and carried-out. The questions of concern are: what's important to patients with this disease? What are the problems that really concern patients? Where are new knowledge and understanding needed? Is a research study designed in a way that patients will respond to? Does the study justify the time and effort patients will put into participating in it? Will it collect the right information, and use it in an effective way? In the end, I always want to help ensure that a study gets at the real issues, and produces relevant information. Sometimes, there are questions of wording too. Medical professionals often use terms in very specific ways, and patients can easily misinterpret them. A patient advisor keeps a watching eye out for this.
I think it is very important, as a patient advisor, to represent all patients, and not just one's own views. After all, we experience this disease in so many different ways, and we deal with it in our own ways. So I talk to fellow patients a lot. I've learnt a few things from this. One is that what's important to patients often isn't what's treated as important in medicine. Life changes in many ways as a disease progresses, and sometimes, the non-medical problems can seem like the biggest ones. Another is that there's a reason we're called patients - it's that we have to be infinitely patient. We often feel like we're spending much of our time, as a fellow patient said, “on someone else's timetable”. Another is that what counts as quality of life in medical research can still leave patients with sizeable day to day challenges. All of these things can inform the advice given by the patient advisor to the research team.
I have also been asked by my hospital to act as 'research champion' for my patient group. This means helping to communicate what's involved in participating in research, encouraging fellow patients to step forward when called on, and answer any questions. Research is crucially important in a number of ways. It produces the information that helps to achieve two goals:
- Better understanding of our needs as patients and carers, so services can better meet them.
- Develop and trial new treatments, behaviours and devices (including both brand new meds, and new ways to use existing meds) - so that genuine progress will be made in how medicine can treat vasculitis and all the knock-on problems that come with it.
I think the most important thing to know about research is this: research is how medicine and healthcare move forward. We, the patients, are the partners of the scientists, medical professionals and other researchers who make it happen. Our role is crucial. Without us, there is no research. Without research, there is no progress.
The patient advisor is there to help this all happen, and that's very rewarding.
How can I get involved?
We are grateful to Vasculitis UK and the Lauren Currie Twilight Foundation for their support with the VOICES study and are committed to involving people with personal experience of vasculitis at every stage. If you would like to offer occasional or one-off advice, or join our advisory panel, please contact Avril Nicoll for more information.
- Study team and funding
-
This study was led by Dr Rosemary Hollick at the University of Aberdeen, in collaboration with Corri Black (Aberdeen Centre for Health Data Science), Louise Locock (Health Services Research Unit, University of Aberdeen), Neil Basu (University of Glasgow), and Mark Little (Trinity College, Dublin).
Dr Warren James was Research Fellow on the data linkage aspect of VOICES, and Avril Nicoll was Research Fellow for the qualitative aspects (Healthtalk interviews and organisational case studies).
The study was funded by Arthritis UK
- Study newsletter
-
We will be producing regular newsletters throughout the course of the study. You can download copies of these newsletters below:
If you would like to be included in the mailing list to receive future issues via email, please contact us at voices@abdn.ac.uk .
- Contact details
-
For further information and enquiries please contact voices@abdn.ac.uk .