What is the background to this study?
Axial spondyloarthritis is a long-term condition of the spine that can cause severe back pain. Symptoms often start in early adulthood and can disrupt education, career and relationships. Up to a third of people with axial spondyloarthritis are estimated to suffer from depression.
People experience and report symptoms such as pain differently when they are depressed, which may influence how doctors assess their response to treatment. One treatment for axial spondyloarthritis is called TNF inhibitors. These drugs do not work in all people. Researchers have sought to find ways of improving response because the number of treatment options for axial spondyloarthritis is relatively limited.
What did we want to find out?
We wanted to see whether depressive symptoms could be linked to how people with axial spondyloarthritis respond to TNF inhibitors. If so, interventions to optimise mental health may help improve response rates.
What did we do?
We used data collected by the BSRBR-AS (British Society for Rheumatology Biologics Register for Ankylosing Spondylitis) to answer our research question. This was a UK-wide study that ran from 2012 to 2017. It collected questionnaires about symptoms of depression and anxiety, along with symptoms of axial spondyloarthritis, from the start of treatment and regularly thereafter.
We compared treatment response between people who reported moderate-to-severe, mild or no symptoms of depression. We then repeated this for symptoms of anxiety.
What did we find?
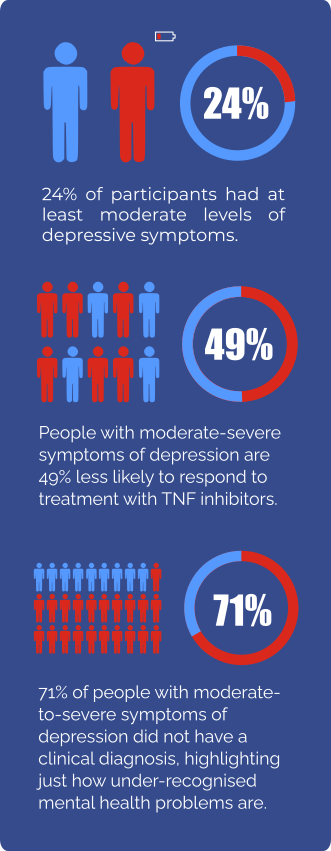
We also found that about 70% of people with moderate to severe symptoms of depression did not have a diagnosis of depression, which highlights just how under-recognised mental health problems are.
Why does this matter?
The size of the potential effect of mental health on treatment response is unparalleled. This makes interventions to optimise mental health very appealing and promising. This is important because mental health conditions are common in people with axial spondylarthritis - commoner than we realise - and because treatment options are limited if they do not respond to TNF inhibitors. Better mental health provisions for axial spondyloarthritis patients are urgently needed.
Who authored this study?
This study was co-authored by Steven Zhao, Gareth Jones, David Hughes, Robert Moots and Nicola Goodson
Who funded this work?
This work was not funded, but the BSRBR-AS was funded by the British Society for Rheumatology (BSR) who have received funding for this from Pfizer, AbbVie and UCB.
Where can I read more?
To view the full scientific paper, click here .
