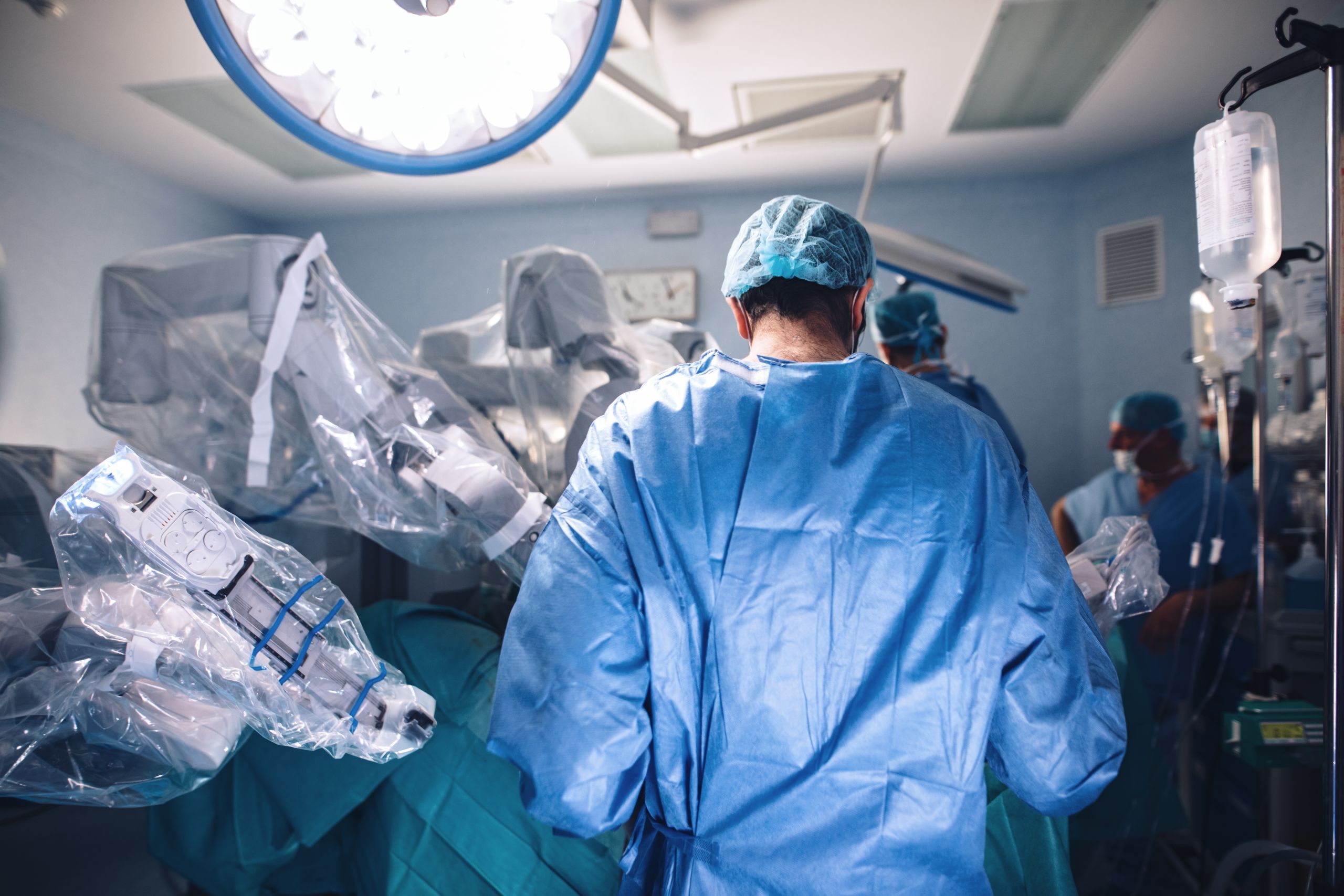
Using robotic surgery to improve patient outcomes
Research is informing new guidelines about the use of robot-assisted procedures to treat prostate cancer.
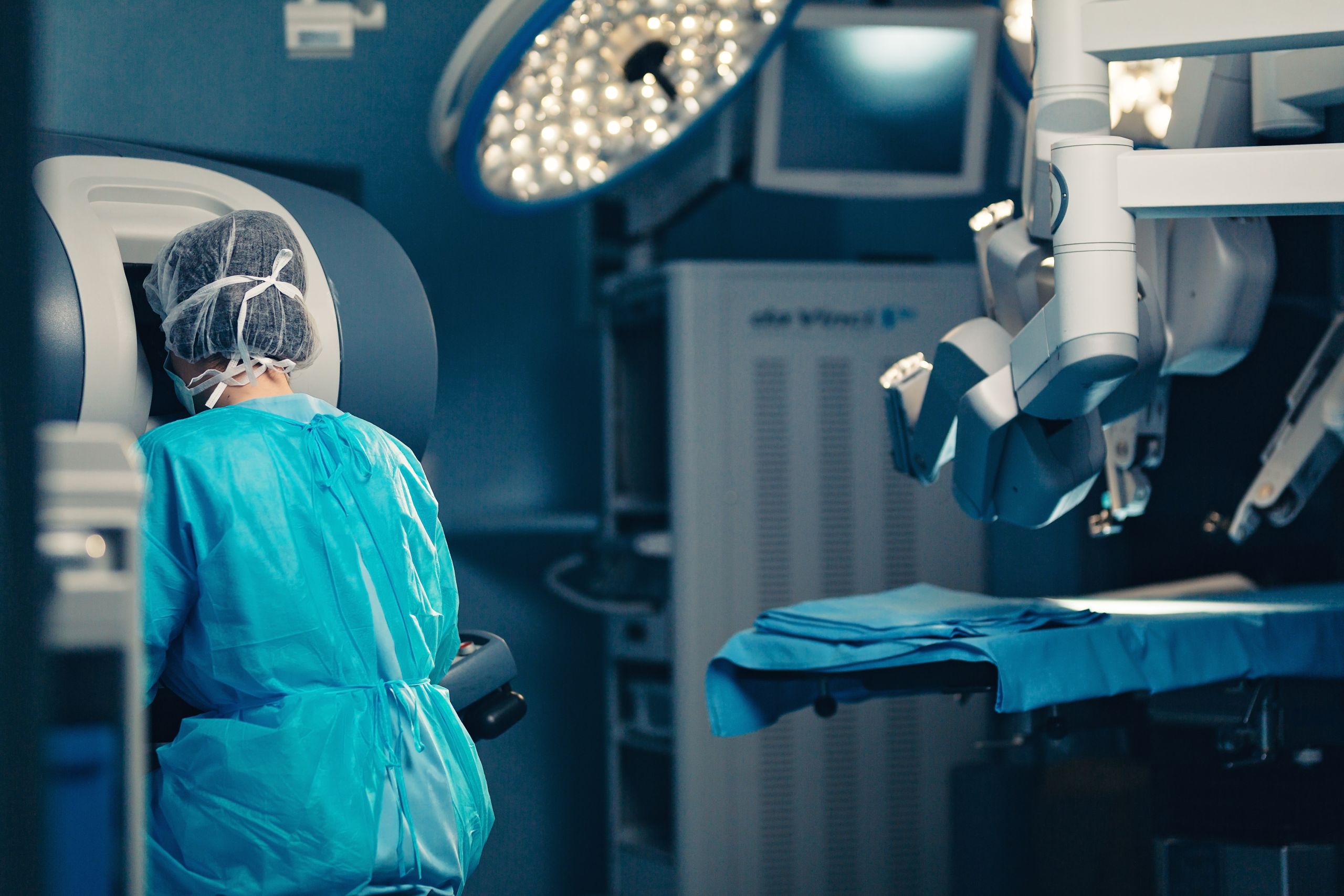
A decade ago, the use of robots in prostate surgery in the UK was limited to a few large research centres, with NICE guidelines focusing on alternative approaches. More needed to be known about both the patient outcomes and the economic case before robot assisted surgery could become more widespread. Researchers at Aberdeen rose to the task.
Prostate cancer is the most common cancer in men. About 1 in 8 men in the UK will be diagnosed with prostate cancer in their lifetimes. Each year, more than 47,500 men in the UK are diagnosed with prostate cancer and 11,500 die, with a further 400,000 men living with and after prostate cancer.
There are a wide range of treatments available including surgery to remove the prostrate, known as radical prostatectomy. Three standard surgical techniques have been developed to carry out this procedure:
1. Open surgery, where the surgeon makes a single large cut in the lower abdomen to reach the prostate
2. Keyhole – or laparoscopic – surgery by hand, where the surgeon makes five or six small cuts in the abdomen and removes the prostate using special surgical tools
3. Robotic-assisted keyhole surgery, where the surgeon uses similar tools as for keyhole surgery by hand, but they control the tools from a console in the operating room via four or five robotic arms.
Initial studies showed that keyhole surgery by hand appeared to offer the potential for better patient outcomes, largely because it is less invasive than open surgery. However, research to assess the place of robotic-assisted prostate removal in routine care were not conclusive, with some demonstrating that robot-assistance might offer improved patient outcomes, such as better removal of all the cancer, and others not showing any benefits. With each robot costing around £1.5 million, the evidence base was not clear enough to justify the investment. Further work was needed to understand the pros and cons.
Evaluating the evidence
A team of researchers, including Craig Ramsay, Director of the University of Aberdeen's Health Services Research Unit (HSRU), set about evaluating the clinical benefits and cost effectiveness of robot assisted surgery. They looked at 57 global studies that compared robotic-assisted prostate removal with other techniques, involving 19,064 patients from 15 countries. They combined this study with comprehensive health economic assessment, using highly specialised economic modelling techniques to understand the case for investment.
Using this combined approach, the Aberdeen team was able to demonstrate that, across the 57 studies, outcomes were better for robotic-assisted removal than for laparoscopic surgery. Not only was there a decreased risk of 30% for major adverse events such as blood transfusion, but failure rates for cancer removal also decreased by around the same amount (31%). The length of time patients needed to stay in hospital was also reduced. Economic modelling proved the cost effectiveness of the approach, indicating that investment in the robot would be offset if it was used for at least 150 procedures per year.

Putting the evidence into practice
The findings of the research were soon being used to inform policy and practice across the UK. In Scotland, a new Healthcare Improvement Scotland evidence note was written, taking the Aberdeen findings into account. This was mirrored in England with updated NICE guidance, which pointed commissioners of urology services to consider providing robotic surgery to treat localised prostate cancer.
As well as medical guidelines, Scottish Government and NHS England were also convinced by the economic case, approving investment to increase the number of robots in use. In Scotland, £3 million was made available by the Scottish Government to invest in robots in Aberdeen, Glasgow and Edinburgh. The first robotic prostatectomy in Scotland took place in Aberdeen in August 2015, and over 1000 procedures have been performed to date. Robots became fully operational in Glasgow and Edinburgh in 2018.
NHS England followed the revised NICE guidelines by implementing a national policy to improve access to robotic–assisted prostate removal for patients with localised prostate cancer. This Clinical Commissioning Policy draws on the Aberdeen research and recommends that robot assisted surgery be offered as a choice alongside existing procedures. Over the past decade, the number of robots being used for radical prostatectomy has increased from 10 to 55. The National Prostrate Cancer Audit report from the Royal College of Surgeons of England show that 89% of prostatectomies in England are now carried out by robot-assistance.
Extending the reach of robotic surgery
Based on these successes, the benefits of robot-assisted surgery are now spreading to other clinical areas and procedures. Once centres have established their robotic skills in radical prostatectomy, they can then train other local clinicians in robotic skills. Members of the research team have continued to provide expert advice, including to Health Improvement Scotland, leading to new guidance on robot-assisted surgical procedures for the diagnosis of head and neck cancer, and treatments for rectal cancer, laryngeal cancers, and renal cancer.
In December 2020, NHS Grampian announced a £5.7million expansion of their robotic programme with the purchase of 3 new robotic machines. One robot will increase the urology treatments available to patients, another is planned for use in knee and hip replacement operations, and the third will be used in general surgery. This signals a major expansion of the benefits of this treatment approach to many more patients in the region.

Impacts
- Aberdeen research has provided evidence for Healthcare Improvement Scotland and NICE, informing new guidelines about the use of robot-assisted procedures to treat prostate cancer.
- The research findings have proved the business case for the substantial investment required for these robots. Over the last decade, the number of robots used for radical prostatectomy surgeries has increased from 10 to 55.
- 89% of radical prostatectomies in England are now carried out by robot-assistance. This has saved time spent in hospitals, shortened patient recovery times, reduced complications, and lessened the physical demands on surgeons.
- By establishing both the clinical and economic basis for using robots, the Aberdeen research has now been extended to underpin decisions in more clinical areas, including other types of cancer, other urology diagnoses, and knee and hip replacement.