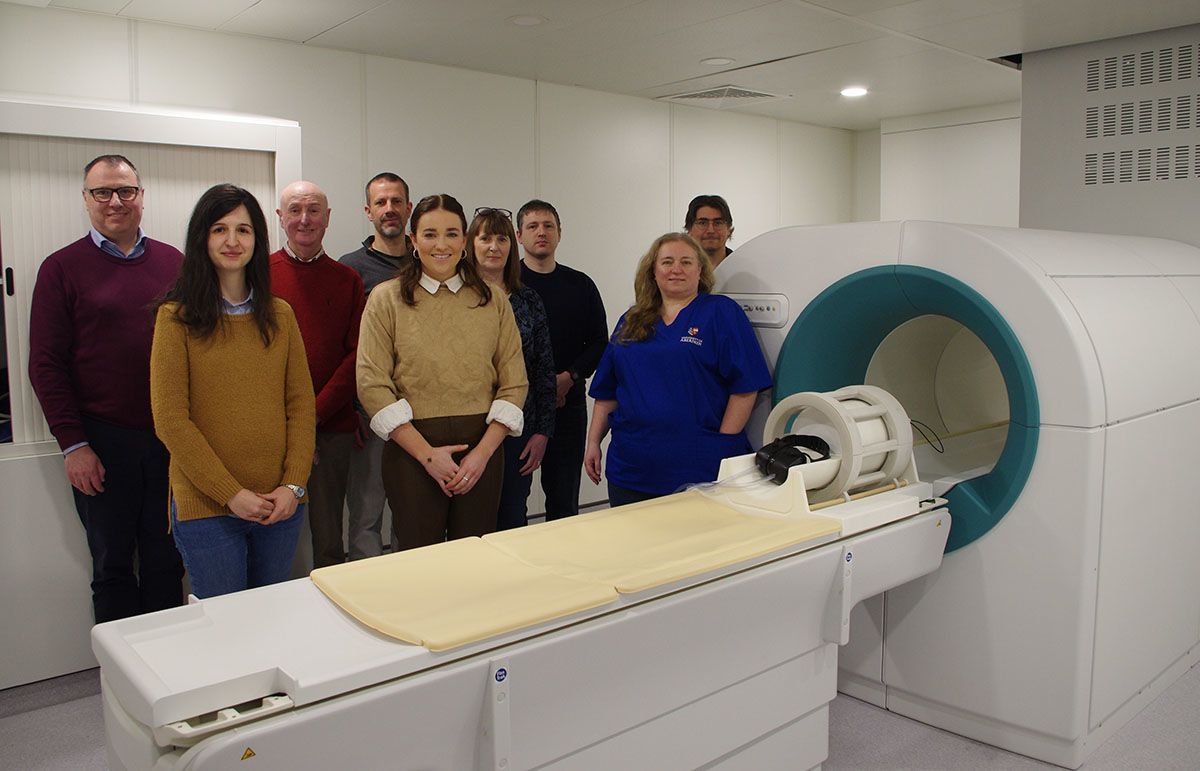
From world first to world leading
How Aberdeen is shaping the future of medical imaging
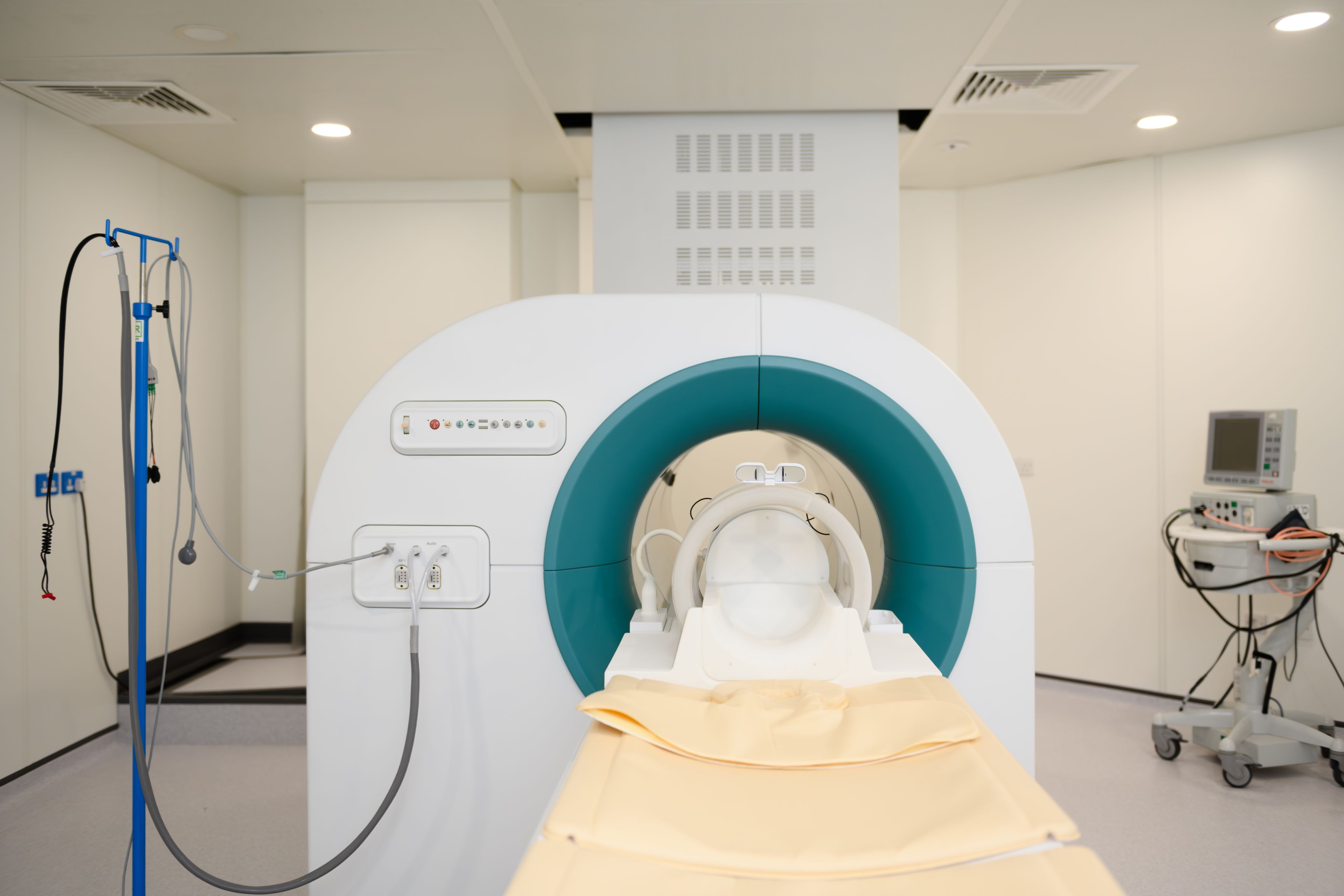
Anyone who has experienced an MRI scan will be familiar with the strange clunking and whirring of the large tube-shaped machines which are a fixture of hospitals around the world.
A strong magnet and radio waves are used to gather signals from the body, and a computer turns those signals into images that doctors can study.
Today we take for granted this technology to enable doctors to see inside the human body. But the story of the first full-body MRI scanner began in a small laboratory at the University of Aberdeen
In the early 1980s Aberdeen researchers – working on a shoestring budget – built and tested a machine which could detect cancer and other changes in body tissue. It was a breakthrough which shaped modern medical treatment.
Four decades on, University scientists are building on that legacy exploring new forms of imaging that could help clinicians detect disease earlier, understand it better and tailor treatments more precisely.
Seeing inside the body
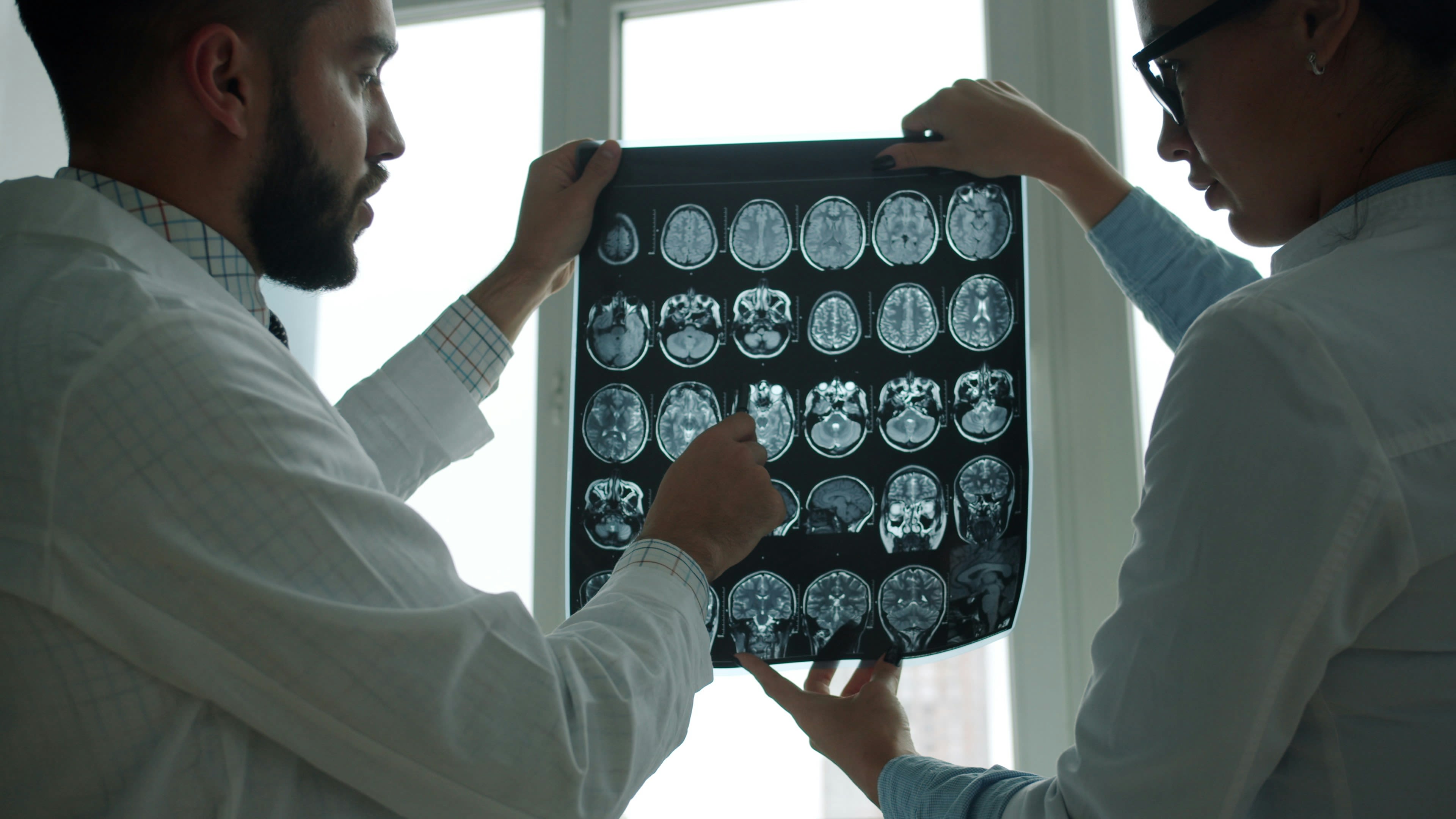
Medical imaging is a simple idea with profound impact: it allows doctors to look inside the body without surgery.
“Medical imaging is any kind of image that helps clinicians make a diagnosis or understand what’s happening inside the body,” explains Dr Lionel Broche, Senior Research Fellow at the University of Aberdeen. “Some images are taken from the outside, like photographs of the skin, but many of the most important ones let us see inside – without having to put anything into the body at all.”
Technologies such as X-rays, CT scans, ultrasound and MRI each play different roles. Ultrasound is familiar to many parents through pregnancy scans. CT scans are often used in emergencies, such as after a suspected stroke. MRI, however, has become especially valuable because of its ability to show soft tissues – organs, muscles, the brain and blood flow – in remarkable detail.
“MRI is extremely good at looking at soft tissue and how blood moves through the body,” says Nichola Crouch, a radiographer working on Aberdeen’s imaging research team.
“It shows where things are in relation to each other, what doesn’t look right and how conditions may be changing over time.”
“Medical imaging is any kind of image that helps clinicians make a diagnosis or understand what’s happening inside the body
Aberdeen’s place in MRI history

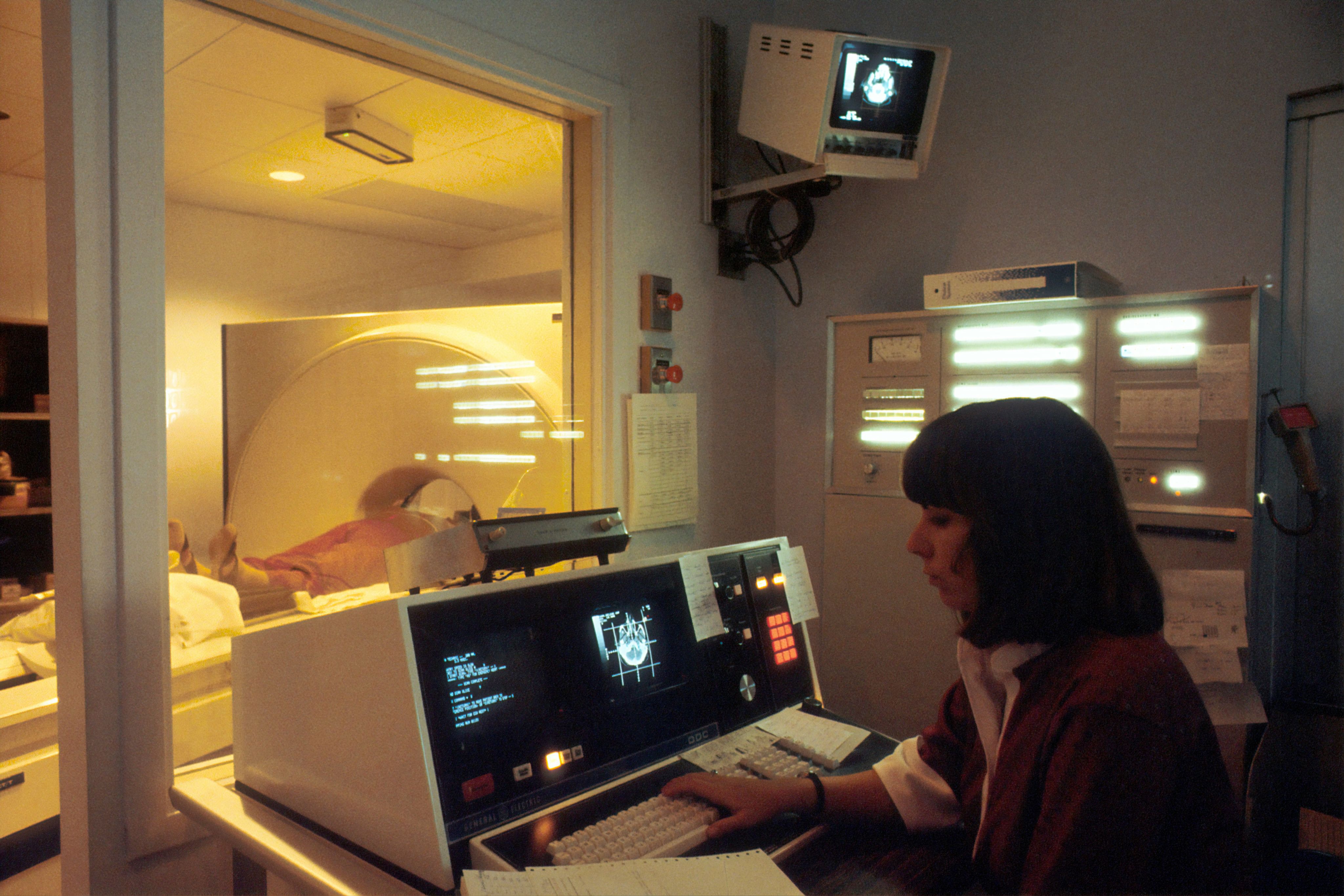
Although MRI scanners are now a common sight in hospitals, when a young researcher named John Mallard arrived in Aberdeen in 1965, the idea that magnetic resonance could distinguish between normal and cancerous tissue was only just being mooted. It was an experimental idea that many experts doubted would ever work as a practical clinical tool.
Under the leadership of Professor Mallard, the University of Aberdeen established one of the world’s first academic medical physics units. His team began experimenting with magnetic resonance techniques, gradually developing a scanner capable of imaging the whole human body.
In 1980, that work reached a historic milestone. The Aberdeen team produced the first clinically useful whole-body MRI image of a patient anywhere in the world. The machine – known as the “Mark 1” scanner – proved that MRI could move beyond small laboratory experiments and into everyday medical care.
“Aberdeen is very famous for MRI,” says Dr Broche. “It has been one of the homes of medical MRI from the very beginning. The first ever clinical MRI scan was made here, and that legacy still shapes what we do today.”
One of the key breakthroughs made in Aberdeen was a technique called spin-warp imaging, which allowed images to be captured more quickly and with fewer distortions. Versions of this method are still used in MRI scanners across the globe, meaning Aberdeen’s influence continues every time a patient is scanned.
Not just pictures, but information
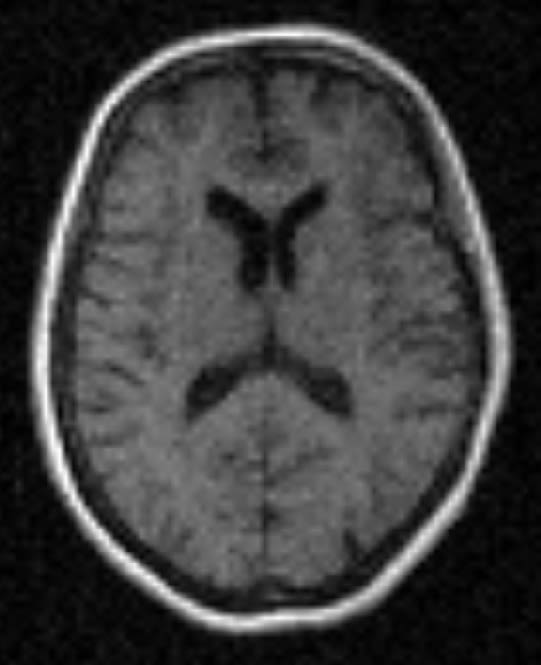
While modern MRI scanners produce incredibly detailed images, Aberdeen researchers are now asking a different question: what information might be hidden beyond the image itself?
That question is at the heart of a new approach known as Field-Cycling Imaging (FCI), a technology being developed and explored at the University of Aberdeen.
Most hospital MRI scanners operate at one fixed magnetic field strength. That single field produces excellent images, but it also limits the type of information that can be gathered.
“With standard MRI, you’re working at one strong magnetic field,” Dr Broche explains. “That gives you great images, but you only see part of the picture. With Field-Cycling Imaging (FCI), we can change the magnetic field during the scan, and that lets us see information that’s completely invisible to conventional MRI.”
He compares the difference to colour.
“Traditional MRI is like having one colour,” he says. “With Field-Cycling Imaging (FCI), you suddenly have many colours. Depending on what you want to see, you can choose the field that gives you the clearest information.”
A scanner unlike any other
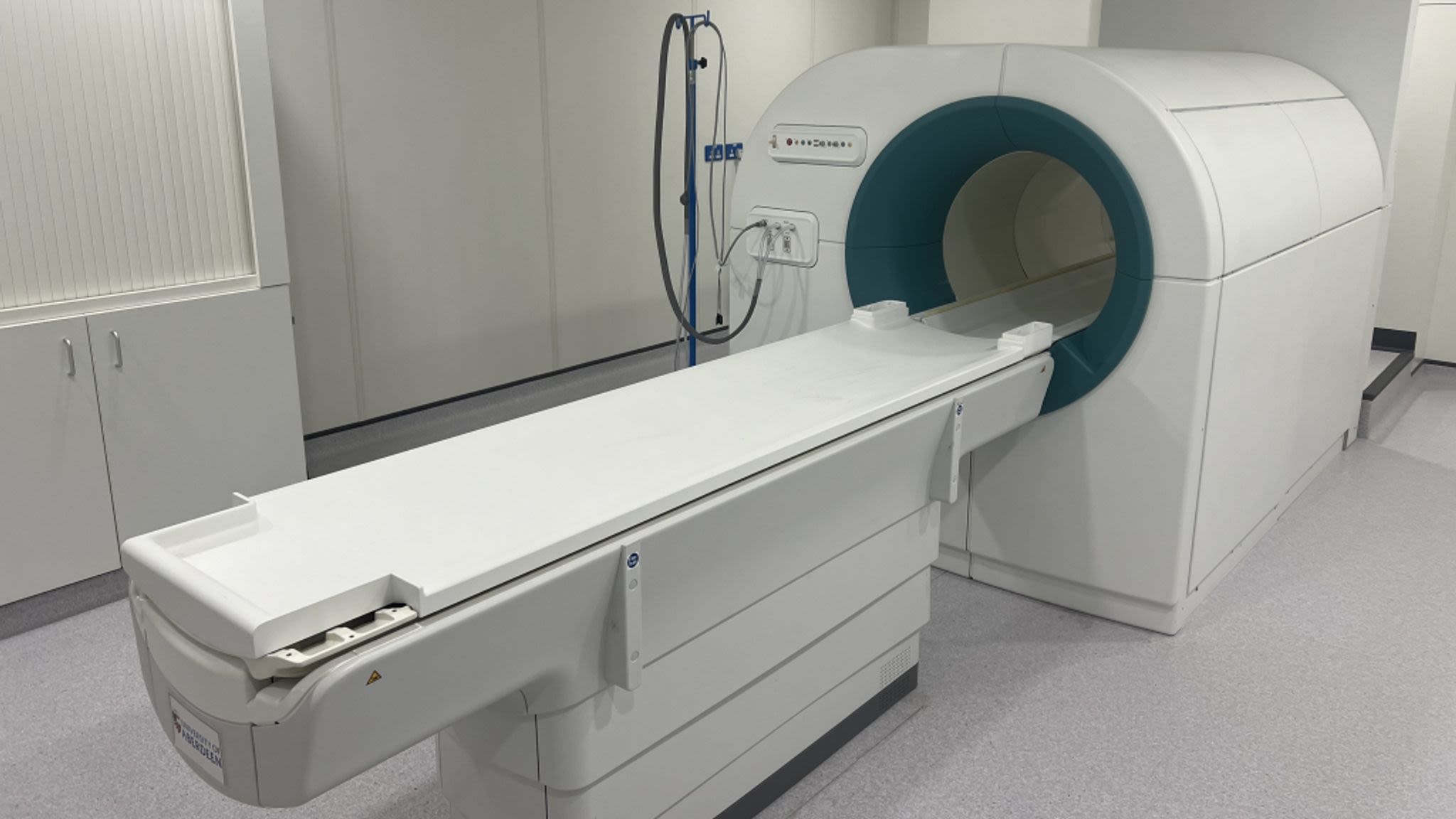
The Field-Cycling Imaging (FCI) scanner in Aberdeen is unique as a system that can scan the whole body while moving through multiple magnetic fields.
“This scanner isn’t about pretty pictures,” says Nichola Crouch. “It’s about background information – what’s happening at a molecular level inside the tissue that you can’t see on a normal scan.”
By utilising low magnetic fields, as well as higher ones during a single scan researchers can observe how molecules – particularly water – move within tissues. These movements can change when tissue becomes scarred, inflamed or cancerous.
“In many diseases, the structure of tissue changes,” Dr Broche explains. “Fibrosis, scarring, tumours – all of these affect how molecules move. At low magnetic fields, those effects become much more visible.”
This means Field-Cycling Imaging (FCI) has the potential to detect disease earlier, to tell different conditions apart, and to monitor how disease responds to treatment.
Early signs, clearer answers
So far, the results are promising.
In stroke research, Aberdeen teams have shown they can distinguish between strokes caused by bleeding and those caused by blocked blood vessels – information that is critical when deciding treatment. They have also been able to identify small vessel disease, a common but often hard-to-detect condition linked to dementia and stroke risk.
In cancer studies, Field-Cycling Imaging (FCI) has demonstrated the ability to spot tumours and even provide clues about how aggressive they might be – without injections or invasive procedures.
“We’ve seen encouraging results in breast cancer, colorectal cancer and other tumours,” says Dr Broche. “We can differentiate tumour tissue from healthy tissue, and potentially see how a tumour is responding to treatment in ways that aren’t accessible with existing imaging.”
Researchers are also beginning studies into osteoarthritis, aiming to detect early changes in joints before irreversible damage occurs.
“We’re hoping to see disease at a very early stage,” says Nichola Crouch. “That’s when treatment has the best chance of making a real difference.”
Research with real patients
Aberdeen’s imaging research is not happening in isolation but is closely linked to clinicians and patients through partnerships with local hospitals.
“It’s incredibly valuable to work with people who actually have the conditions we’re studying,” says Crouch. “Patients, clinicians and researchers are all part of this process, and everyone understands that what we’re doing now could shape care in the future.”
Patients who take part know the technology is still at the research stage, but many are motivated by the possibility of helping future diagnosis and treatment.
Building on a proud legacy
From the first full-body MRI scan in 1980 to today’s exploration of field-cycling technology, the story of medical imaging in Aberdeen is one of curiosity, persistence and ambition.
“What we’re doing now is building on that original breakthrough,” says Dr Broche. “We’re continuing to ask how imaging can tell us more – not just where disease is, but what it’s doing and how it’s changing.”
And developments in Field-Cycling Imaging (FCI) are not the only way in which the institution is contributing to the future of medical imaging. A research team working in parallel is leading exploration of Low-Field MRI which offers further benefits in cost, accessibility and patient experience.
The answers may take years to fully emerge but research from the University of Aberdeen could once again help transform how medicine sees the human body.